Project Fed | Exclusive Pumping + (Mostly) Hating It
A few weeks before I started this project I met Kelly and Hazel at Hazel’s newborn session. We commiserated briefly then about the latch, tongue tie, and maternal health issues that forced Kelly to abandon the goal of breastfeeding and take up pumping exclusively. As of our newborn session it seemed like they were in a good place, but matters continued to devolve.
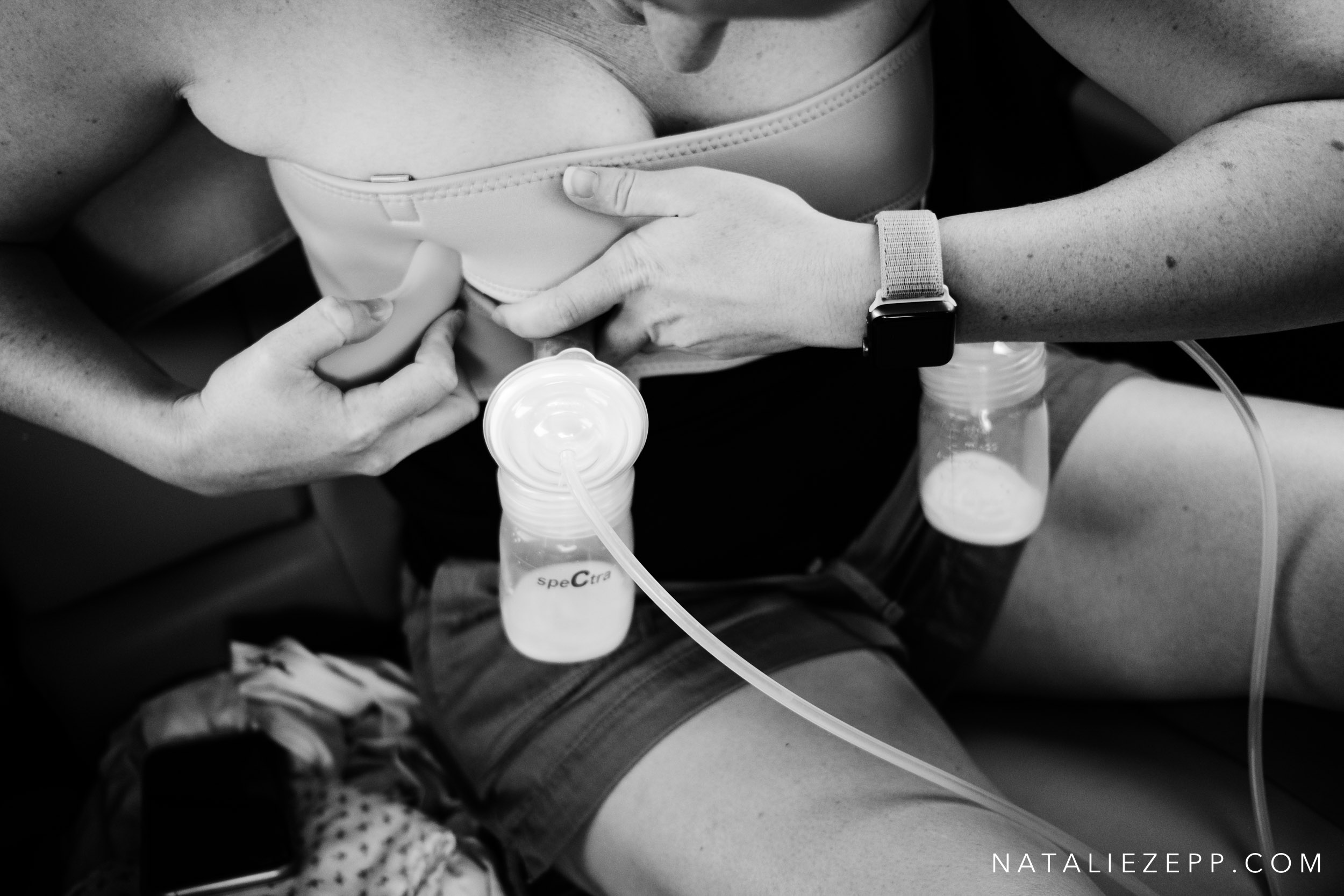
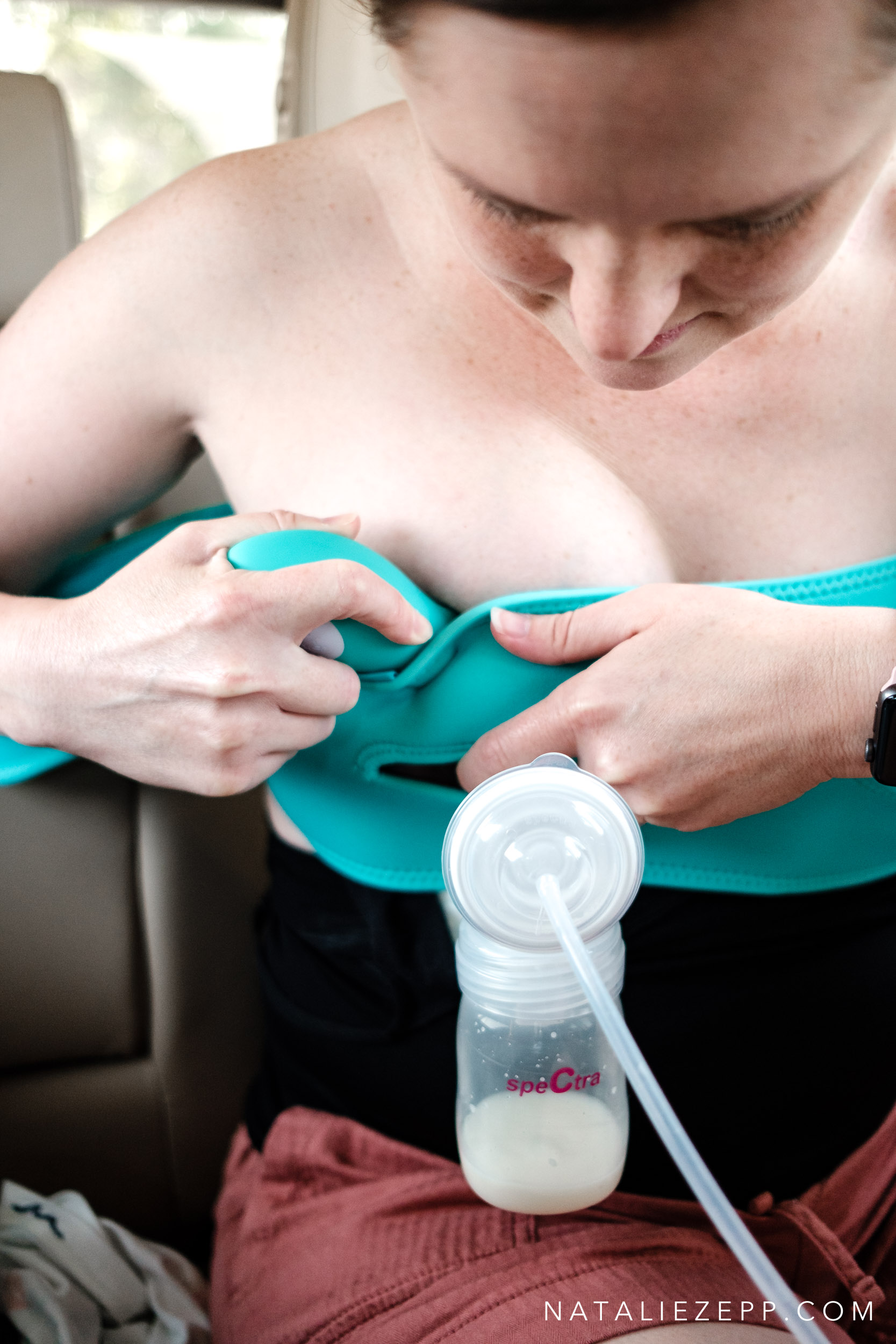
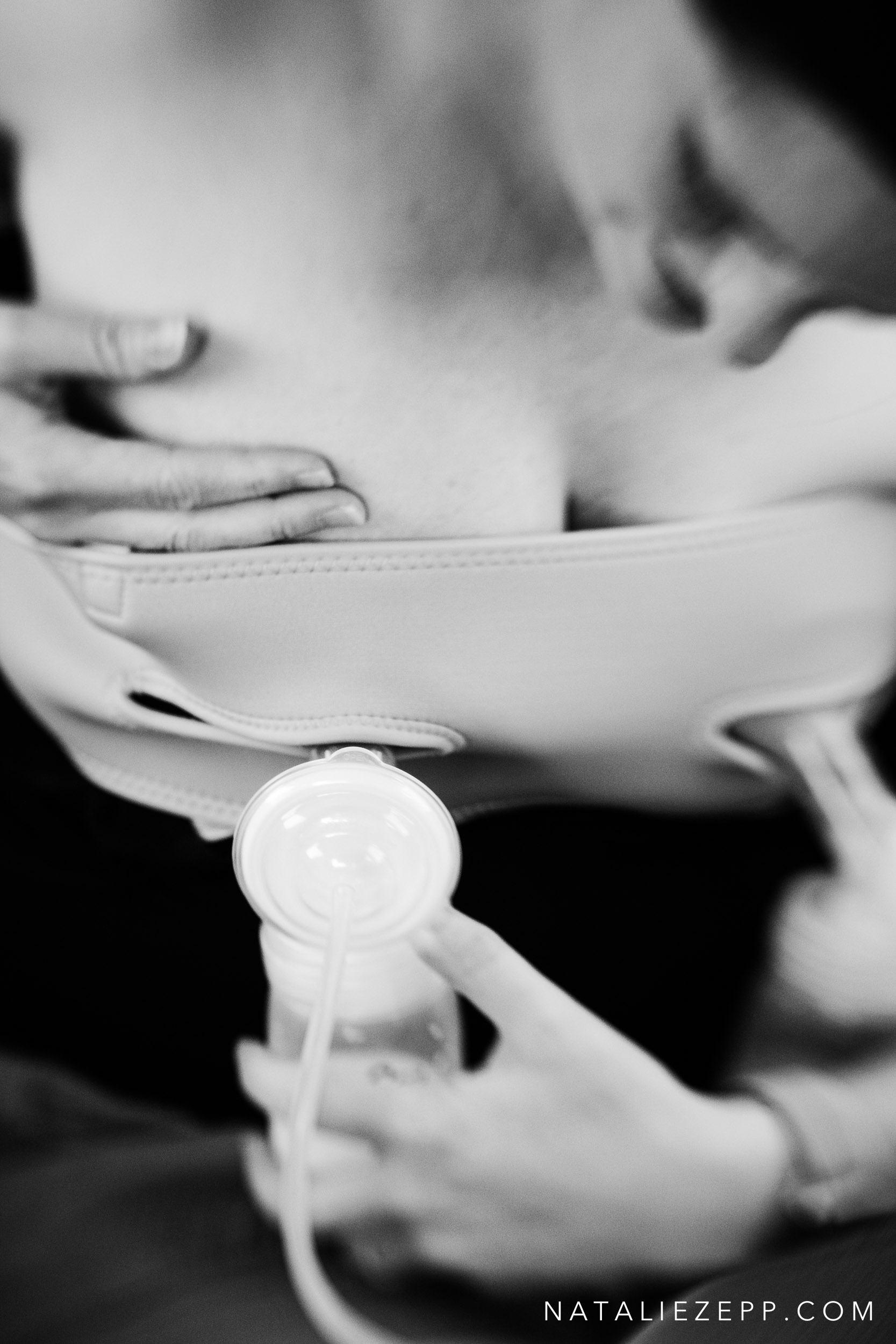
The morning we were to meet for our Project Fed session, Kelly texted me to what a perfect day it was for this, because she could feel another clogged duct coming on and was feeling really down about it. The entire time we sat in her car (her favorite place to pump and still be with the family) and chatted, she pumped while ferociously assaulting her breast with a handheld massager in an attempt to break up the clog and prevent another round of mastitis. Kelly lamented that she is ‘so done’ with pumping so aggressively. She would love to stop and just spend what is left of her maternity leave enjoying the precious time with her daughter.
Unfortunately, the only cure for these clogged ducts is to continue to pump. Which only increases supply, making it even harder to stop without suffering more clogged ducts! It’s a vicious cycle that she can’t seem to escape. Still, thru all of the pain and struggle, Kelly never fails to seem positive and grateful for the way that this experience has deepened her love for her husband and strengthened her marriage.
Here is Kelly’s story in her own words:
“My daughter, Hazel, was born on April 15, 2019. While at the hospital, we had many folks watch us breastfeed to make sure we were getting the hang of it. It seemed like we had the normal struggles, but we were getting the hang of it overall. Hazel wouldn't latch for a long time. So to make sure she was getting something, we would hand express into a small cup and then feed her the expressed colostrum with a spoon. At the time we were concerned because everything coming out of my right breast was an extremely dark color, but we were told by the lactation consultant that it was normal. Later we would be told that I had "rusty ducts". As we were about to leave the hospital, the lactation consultant did an inspection of Hazel's mouth and determined that she could have a tongue tie. We decided that we'd reevaluate at our 4 day weigh-in.
Before we even left the hospital, I was starting to show signs of spinal headaches from the epidural, but the nurses had assessed that it was simply a tension headache from exhaustion and the construction in the hospital. By the next day, they were full blown migraines that earned us a visit to the ER (with a 3 day old baby). They didn't want to give me a blood patch, but instead recommended that I drink a ton of caffeine (no kidding, go home and drink a Monster), and the headaches will for sure go away in 1-2 weeks. Naturally, they lasted the full 2 weeks. This was completely debilitating for me, making it hard to feed Hazel. My body was already so stressed that I kept feeling like it was transferring over that stress to her making it hard for her to feed.”
“When we returned to L&D 4 days PP for Hazel's weight check, she had lost 11.5% of her birth weight (flagging an issue at 11%). At that time we had a pediatrician evaluate her tongue tie, which he determined to be a severe one. We elected to have it cut at that time, and were told that we'd basically be starting over with breastfeeding for the next few days (cluster feeding, etc.). When we got home, things certainly weren't fantastic...lots of crying (so much that she went hoarse) and some long latches that seemed unproductive. I was talking to the lactation consultant the whole time, even sending videos to see if we were doing everything correctly. She had even sent us home with a small syringe to place in her mouth while breastfeeding to get her a little extra milk (that had been previously expressed). When we returned for another weight check and 6 days postpartum she had lost 16% of her birth weight. We went into full panic mode, immediately feeding her formula and then weighing her to make sure it wasn't another issue. Then they attempted to get an IV in her for 4 or 5 hours, pricking her nearly a dozen times before they finally succeeded. We were admitted at that time and stayed for approximately 36 hours until the doctors felt good about her weight gain, only feeding her expressed breast milk and formula. I was still experiencing epidural headaches the whole time we were at the hospital, making it very difficult when staff continued to come in and turn the lights on (which I was very sensitive to) and the obvious stress/exhaustion. Once we got home, breastfeeding was straight out. We gave her as much breast milk as possible and supplemented with formula until my supply was high enough. By a week later (2 week PP) she was finally above her birth weight and gaining steadily! We were in the clear. At least for Hazel. We were referred to an infant feeding therapist to get more answers. Turns out her tongue tie was severe enough that even in utero when she was practicing sucking, she was overcompensating with how far she'd open her mouth up, therefore making her jaw strength extremely minimal. So she never developed the strength or endurance to breastfeed, which is why she could be latched for so long but not get anything out of it. We were able to learn some exercises to get her back to the breast, but unfortunately I was hit with a number of infections around the time we would have started that. Now we've fully committed to pumping breast milk and feeding her with the bottle.”
“About 2.5 weeks postpartum, I was overcome with immense pain in my lower abdomen and back, so bad that I was crying in pain and my husband had to carry me to the shower. The running hot water was the only thing we could think of to ease the pain. Luckily I had some oxycodone to hold me over to the next day. The next day (Friday) I was able to talk to one of the nurses at the clinic to get an antibiotic course started for a UTI over the weekend. I went in for a urine sample, but we were confident at the time it was a urinary tract infection. By Sunday, I was feeling better in terms of the UTI, yet worse in other ways. I had started getting a number of flu symptoms including chills, fever, sensitivity, and a cold sweat. The same day I noticed a lump starting to form in my right breast. First thing Monday morning, I was on the phone with the clinic again getting a same day appointment set up. Textbook mastitis…you’ve got to be kidding me. And on top of that, the antibiotic I had taken over the weekend for the UTI was resistant to my string of infection. At this point, they had to determine which infection to fight first. They gave me a one-time dose of antibiotic for the UTI, and then I was to start a 10-day course of another one the next day for the mastitis. The day after I started the antibiotic for the mastitis, the midwife called back to tell me that they gave me the wrong dosage AND that my OB didn’t like that antibiotic for my case, so I was placed on a fourth antibiotic in 5 days. I ended up experiencing flu symptoms for about 5 days.”
“I became very aware of my tendency to get clogged ducts. At one point I developed a mass the size of a baseball in the same spot of my mastitis, near the end of my antibiotic course. I had tried it all, taken all the suggestions from my mom friends, OB, midwives, lactation consultant…even Dr. Google. In the end the only thing that worked for me was taking a massager to the lump after a scorching hot shower localizing the water on the affected area of the breast. I took a lot of hot showers that week. Understandably I started having cracked nipple issues causing lots of pain while pumping. It took weeks, but my supply recovered and I continued to learn how to care for my precious boobies (coconut oil is the best). They had just been beat up!
Nearly 7 weeks PP, and I was in my stride. I was pumping 42 ounces a day! I even rented a hospital grade pump since I am exclusively pumping. I moved away from pumping every 2-3 hours and managed to make it to 4-5 hours. Quality of life was up! I finally felt like I could do this, this huge challenge I was faced with. I was finally conquering it. Then, just like the cruel joke that has been my whole postpartum experience, I get hit with thrush. I can’t believe it. How on earth is this even possible?! I sanitize all my parts every time, I go boobies out constantly to keep those suckers dry, I keep them clean…I don’t get it. Thank goodness the baby doesn’t have it and hopefully it’ll stay that way. Now everything that comes from that breast is trash. Whoever came up with the term “Don’t cry over spilled milk” clearly isn’t a pumping mama.”
“So here I am, 10 weeks postpartum and I feel like I’ve experienced every issue in the book. Pumping is a whole different labor of love. I’m still navigating how to do it all. When I imagined what this time would look like, I thought I’d be sore the first few weeks from my 3B tear. I knew I’d be burdened with body image issues as I struggled to lose all the weight and got used to all my new “birth marks”. Sleepless nights, crying baby…totally, we can handle that. But all this extra stuff, no I did not expect it. Between the epidural headaches, UTI, and then the mastitis, I wasn’t able to care for my daughter for most of the first month of her life. My husband exclusively cared for us, making me fall in love with him even more than I thought was ever possible. He ended up taking even more time off work, which was necessary in every way. When I felt good enough, I would get jealous of the time he was spending with her. I felt like I wasn’t getting to know her as much as he was. But I have to remember that everything is temporary, even though it feels like my issues are never ending. Am I upset that we’re bottle-feeding, absolutely not. Fed is best. I am so happy that my baby knows a full belly and is continuing to grow into a beautiful and fun little girl. I will say that we have to stop saying things like "we couldn't figure out breastfeeding" like we're not smart enough. That's BS. Breastfeeding simply didn't work for us, and that's okay!"
“As much as our situation has sucked, in many ways I’m grateful that this happened to us and hopefully not someone else. We are blessed with endless resources to help us get through these challenges. Not everyone is that lucky. But I will say, I really hope this postpartum amnesia is a thing. I love my child more than I could possibly explain. Yet this experience has really scared me from wanting to be pregnant again. I'm not sure if we'll continue pumping anymore. I want to so badly, but I don't think I can handle another infection. Still to be determined. For now, I'll continue to be entertained by my purple stained boobies from the Gentian Violet in hopes it will kick this infection before the doctors put me on my fifth antibiotic.”
Kelly has continued to update me on her pumping journey since our session. She had more experiences and perspective to share on subsequent challenges of traveling while exclusively pumping, returning to work, and the bittersweet decision to stop pumping. We’ll continue with her words:
“Many things have changed since I previously wrote about my journey 10 weeks ago. Now at 19 weeks postpartum, for better or for worse, I am officially done pumping. We’ve had many guests visit us, some that I didn’t want to pump in front of. We’ve gone on 7 airplane rides with Hazel, some clear across the country. And I returned to work…pumping through all of that. I can say with confidence that pumping can be a very lonely journey that society has not figured out how to handle yet, but we’re getting there.
Often while we had guests I would pump in my bathroom sitting on the edge of my bathtub totally uncomfortable in effort to not make my guests uncomfortable. It’s not a big deal when you maybe pump once a day, but when you pump as often as your baby eats, it adds up. I’d often have to remind myself that this is my house, but more importantly I’m providing for my child and I don’t need to care about anyone else but her in that moment. As a people pleaser, this was difficult.”
“Flying commercial was a whole different puzzle. Normally parents are trying to time out feedings and how much milk to bring. We were adding the puzzle piece of when exactly to pump to maximize our time and not run out of milk during our travel. Or which milk should we use first, the cold milk that has to be used within an hour after it’s warmed up, or the milk I just expressed? How long is that good for…4 hours...now when will that be…which leg of our trip is that on…oh shoot now we’re delayed?! The fun was endless. Once, we had the joy of being able to use one of the pumping pods at a larger airport because we had just enough time between flights. What a DREAM! But the stress of having to figure out your feeding and pumping schedule while traveling with an infant is just incredible. I am so glad that we did it, but sometimes I wonder how we managed.
Then there was going back to work and the inevitable weaning that had to follow. My first day back to work I asked where I could pump at lunch. The bathroom was recommended. I politely replied that is a poor option for sanitary reasons and everyone quickly understood. We never quite found a good solution, but we found a solution. Luckily my employer is coming around to putting standards in place to give pumping mothers access to safe and sanitary locations at their workplace. But again, pumping was lonely and took so much time. Time that I could have been eating, because guess what…when you’re an overproducer and have to really focus on your pump, you can’t eat at the same time. You can’t do anything at the same time. Then there is setting up the pump, cleaning your parts, putting everything away. You’ll be lucky if you can make that whole turn in 25-30 minutes.”
“I lost so much of my time to my pump. Think about it. Even if you only pump three times a day, and you add in the time to set it up and wash your parts, you lose minimum of an hour and half in your day. That’s time away from chores, making dinner, your job, quality time with your spouse, precious moments with your child, or heck…nothing at all. Because let’s be honest, just sitting is extremely important for your recovery as a new parent too. But then there is so much emotion tied to pumping. It’s this labor of love that you’ve put so much of your life into that weaning is hard and painful! Not just physically, but emotionally. I took my time. It wasn’t just a few days or a week like some people will tell you, for me it took weeks. I cried, I felt like I was losing a part of myself, a part that I was so completely fed up with yet I wasn’t ready to say goodbye too. My choice to stop was for many reasons that I never need to explain and all of them made more than enough sense. But it was still very sad to end that chapter.
What a journey! I learned a lot in the process. Exclusively pumping is a whole different labor of love that many don’t understand. Pumping is lonely and confusing. Explaining your need to pump to your employer is awkward. You don’t need to defend how you feed your baby. You’re keeping your baby alive, healthy and happy whether that’s from your breast, expressed milk, or formula.“
What piece of advice or encouragement would Kelly give to another struggling mom?
“You are doing so great mama and most importantly, you are not alone! Lean on your partner because that’s what they are there for and they want to help. Reach out to other moms, the experience they’ve had could help. Ask for help early and often, if you wait it could only make your issues worse. You are not a burden. You are a superhero. And what you are doing as a mom to raise your beautiful child is the greatest gift you’ll ever give.”
Project Fed is a photojournalism project inspired by the stories of mamas struggling physically and/or emotionally with feeding their baby. Do you have a story to share? It seems most of us do. I’d love to hear yours. Share in the comments or click the button below to read more details about and/or participate in Project Fed. Thank you!